|
This study is part of the ISAR-study, which is registered at (identifier number: NCT01152892, URL: ). Patients, inclusion and exclusion criteria Hence, the aims of our study were to examine the overall degree of dementia in this patient population for the first time using the CDR and to reevaluate cut-off values for the MoCA test to distinguish cognitively normal and impaired hemodialysis patients. 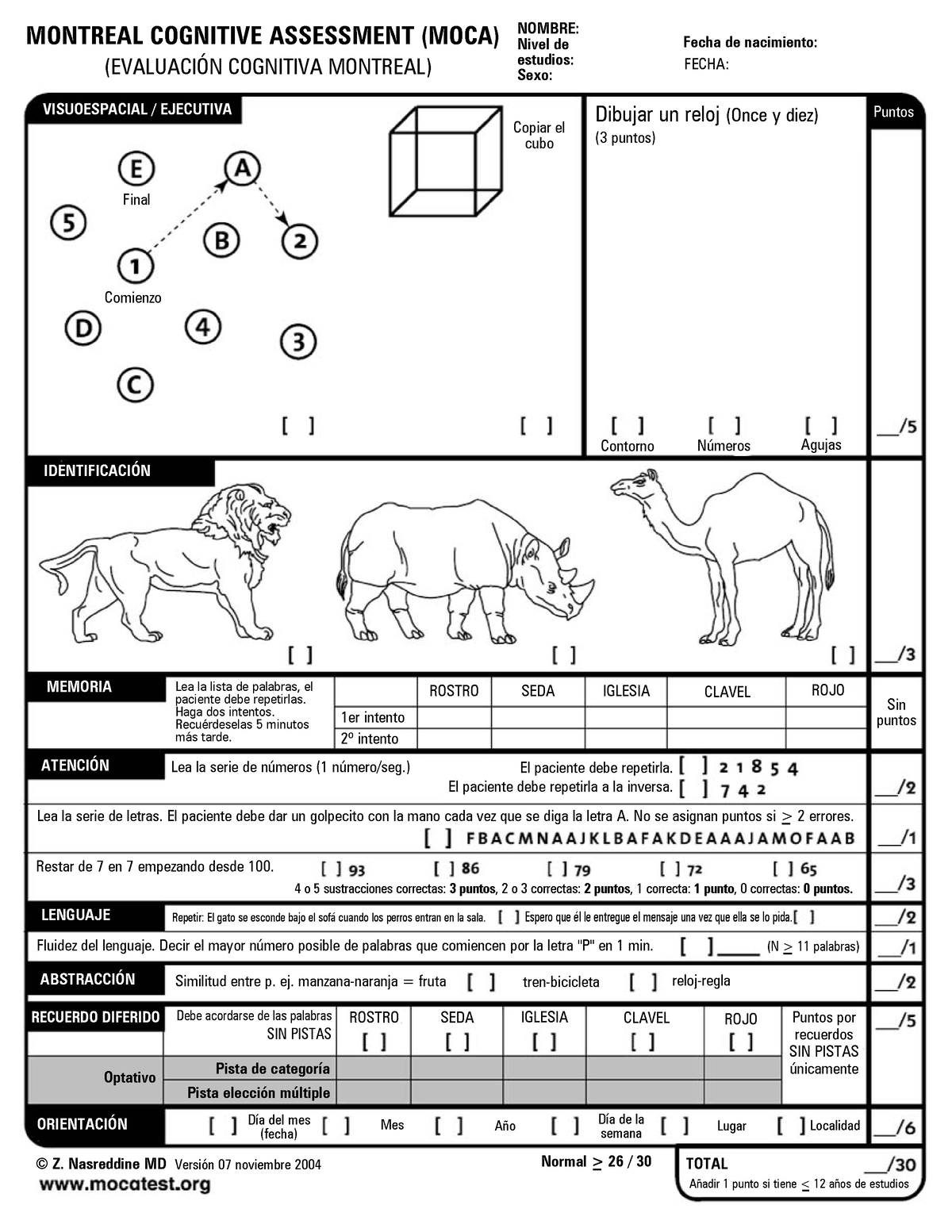
Despite its important role in evaluating the degree of cognitive impairment independent from the underlying condition, the CDR has never been applied in hemodialysis patients before. The Clinical Dementia Rating scale (CDR) is an international standard to assess the overall severity of dementia taking both cognitive symptoms and impairment in activities of daily living into account by interviewing the patient and his informant or caregiver. Īccording to the Diagnostic and Statistical Manual of Mental Disorders (DSM)-IV and the International Classification of Diseases (ICD)-10 guidelines the diagnosis of dementia is based on the presence of cognitive impairment and consequently an impairment of daily activities and independence. Only one study validated a short screening instrument, the MoCA, identifying a cut-off of 24 points to be more suitable to detect cognitive impairment compared to the established value of 26 points. 
In previous studies in hemodialysis patients the Montreal Cognitive Assessment (MoCA) test, the Mini-Mental State Examination (MMSE) or the 3MS have been applied using established cut-offs. In this context, a short screening instrument is the most resource-efficient option, which has to be precise in identifying impaired patients as well as those in need for further evaluation. Thus, periodic screening is needed to identify patients with relevant cognitive impairment in order to improve their clinical care as well as to reduce health care costs. Moreover, dementia is associated with disability, hospitalization and an approximately 2-fold increased risk of both dialysis withdrawal and death. Educational level had a significant impact on MoCA scores.Several studies demonstrated high prevalence of cognitive impairment in hemodialysis patients as well as its potential adverse effects on management and outcome including interference with informed decision making, capacity for self-care and adherence to medical, fluid and dietary instructions. Conclusions: Approximately 50% scored below the cut-off score of 26 points, suggesting that the cut-off score may have been set too high to distinguish normal cognitive function from MCI. Those with higher education had significantly higher scores (mean 26.2, 95% CI 26.1–26.3 vs. The mean MoCA score was 25.3 (95% confidence interval 25.2–25.4), and 49% had a score below the suggested cut-off of 26 points. Results: MoCA scores were available in 3,413 participants, of which 47% had higher education (>12 years). The participants were aged 63–65 at the time of data collection. Methods: MoCA scores were assessed in the Akershus Cardiac Examination 1950 Study, a cross-sectional cohort study of all men and women born in 1950 living in Akershus County, Norway. AbstractAims: To investigate Montreal Cognitive Assessment (MoCA) test scores in a cohort aged 63–65 years from a general population in relation to the proposed cut-off score of 26 for mild cognitive impairment (MCI) and to explore the impact of education.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
